Melasma: What are the best treatments?
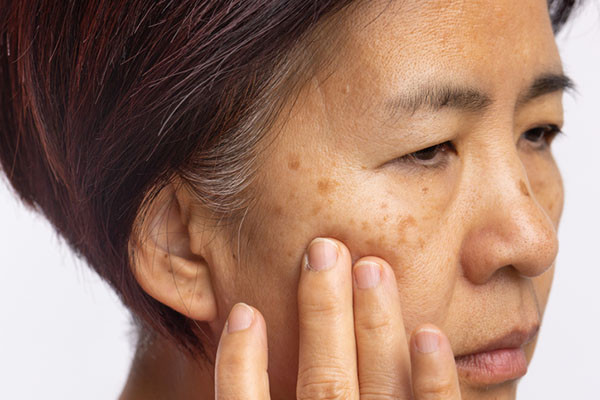
Melasma is a pigmentation disorder of the skin mostly affecting women, especially those with darker skin. It is commonly seen on the face, and appears as dark spots and patches with irregular borders. Melasma is not physically harmful, but studies have shown that it can lead to psychological problems and poorer quality of life due to the changes it causes in a person's appearance.
Melasma is a common disorder, with a prevalence of 1% that can increase to 50% in higher-risk groups, including those with darker skin. Melasma is known as the "mask of pregnancy" since hormonal changes caused by pregnancy, as well as hormonal medications such as birth control pills, are major triggers for excessive skin pigment production in melasma. Sun exposure is another important contributor to melasma.
Can melasma be prevented?
Currently, melasma cannot be fully prevented in people who are likely to develop this condition due to their genetics, skin color type, hormones, or sun exposure level. Avoiding direct sun exposure during peak hours (10 a.m. to 4 p.m.), diligently using high-SPF sunscreens, and avoiding hormonal medications when possible may help protect against melasma flares and reduce their recurrence after treatment. Strict sun protection is the mainstay of any melasma treatment regimen.
What sunscreen should melasma patients use?
Choosing an appropriate sunscreen is critical if you develop melasma, and studies have shown that broad-spectrum tinted sunscreens, especially ones containing iron oxide, can lower pigment production in the skin in melasma patients, as they block visible light as well as UVA/UVB rays. Non-tinted sunscreens, on the other hand, do not block visible light.
For some people, it might be more convenient to use cosmetic products such as foundations that contain both UVA/UVB blockers and visible light blockers such as iron oxide. These products can conceal dark spots and therefore alleviate the psychosocial impact of melasma, and at the same time act as a sunscreen to protect against darkening of the lesions.
It is important for people with melasma to know that visible light can go through windows, and therefore even if they are not out in the sun, they can still get melasma flares by exposing themselves to visible light while driving or sitting by a window.
Can melasma be treated?
Currently there is no cure for melasma; however, there are several medications and procedures available to manage this condition. It is important to know that these treatment options may result in an incomplete response, meaning that some of the discolorations become lighter or disappear while some remain unchanged. In addition, frequent relapses are common.
It is also important to be aware of possible side effects of treatment, including darkening of the skin caused by inflammation induced by the treatment, or extra lightening of the skin in a treated area. Using the appropriate medications under the supervision of a dermatologist can help achieve treatment goals and maintain them with fewer relapses.
Common melasma treatments
The most commonly used treatments for melasma are skin lightening medications that are applied topically. These include medications such as hydroquinone, azelaic acid, kojic acid, niacinamide, cysteamine, rucinol, and tranexamic acid. These medications work by reducing pigment production and inflammation, and by reducing excess blood vessels in the skin that contribute to melasma.
Pregnant women (who constitute a big proportion of melasma patients) should avoid most of these medications except for azelaic acid, which is a safe choice during pregnancy. Hydroquinone is a commonly used skin lightener that should only be used for a limited time due to side effects that may happen with prolonged use. It can be used for up to six months for initial treatment and then occasionally if needed.
In most patients a combination therapy is needed for treatment for melasma. A common choice is the combination of hydroquinone with a retinoid that increases skin cell turnover and a steroid that decreases skin inflammation. Oral medications, including tranexamic acid, are usually considered in more severe melasma cases. This medication is thought to help melasma by reducing pigment production and by reducing excess blood vessels in the skin.
Additional treatment procedures may help
If your melasma does not improve with topical or oral medications, adding procedures such as chemical peels and laser therapies to a treatment regimen could be beneficial.
Chemical peels use substances like glycolic acid, alpha-hydroxy acids, and salicylic acid to remove the superficial layer of the skin that contains excess pigment in melasma patients. The effects of a chemical peel are temporary, since this procedure removes a layer of skin without reducing the production of pigment in regenerating deeper layers.
Laser therapies can destroy pigment cells in skin and therefore lighten the dark spots in melasma. However, as with any other treatment option for melasma, there is considerable risk of relapse post-treatment.
Maintenance therapy and prevention
After achieving improvement of melasma lesions, strict sun protection and maintenance therapy need to be continued. Skin lighteners other than hydroquinone can be used in combination with retinoids to maintain the results, and hydroquinone therapy may be used intermittently if needed.
Takeaway message about melasma
The key point in management of melasma is to use sun protection all the time, and to avoid other triggers such as hormonal medications when possible. Since none of the available treatments are a cure, prevention is the best option. People with melasma should see a board-certified dermatologist for evaluation and appropriate treatment regimens to manage melasma and maintain the treatment results.
About the Authors

Lilit Garibyan, MD, PhD, Contributor

Sara Moradi Tuchayi, MD, MPH, Contributor
Disclaimer:
As a service to our readers, Harvard Health Publishing provides access to our library of archived content. Please note the date of last review or update on all articles.
No content on this site, regardless of date, should ever be used as a substitute for direct medical advice from your doctor or other qualified clinician.