How high blood pressure harms your health

Time for a medication check-up?

Risk factors for MCI and dementia

Handling tough decisions as a caregiver

How we make memories

Treating mild cognitive impairment

Are you at risk for high blood pressure?

Cholesterol's various forms

Stopping a medication?

How to fall without injury
Breast Cancer Archive
Articles
Toxic beauty
Are your personal care products putting your health at risk?
The average woman uses 12 different beauty products every day — cleansers, conditioners, hair dyes, fragrances, skin care products, scented lotions, nail polish, and makeup, to name a few. Take a quick glance at the labels, and you'll see a cocktail of chemical components.
You might assume that all these ingredients have been tested to ensure that they're safe for long-term use. That's not the case.
Researchers test new technology for screening dense breasts
Research we're watching
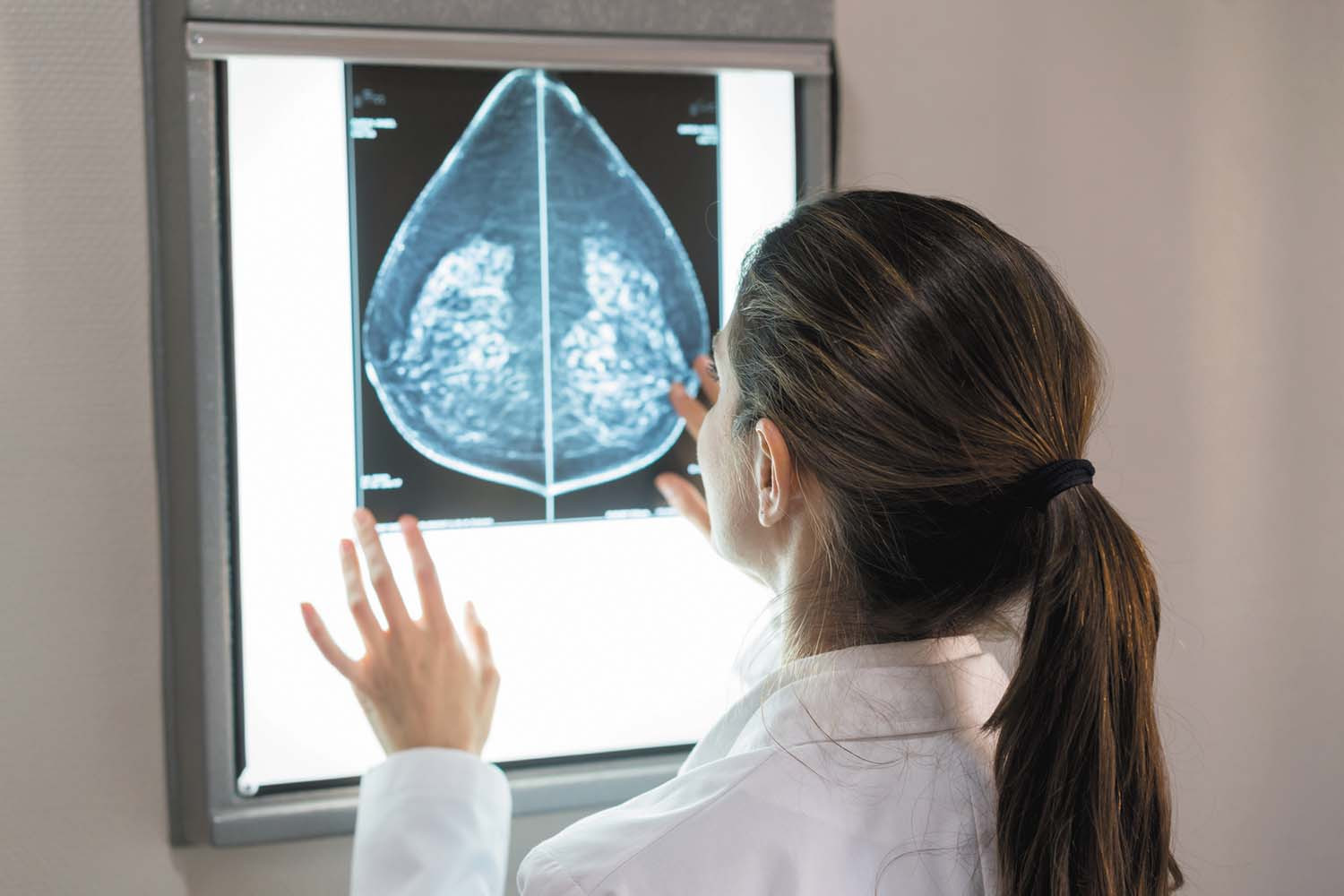
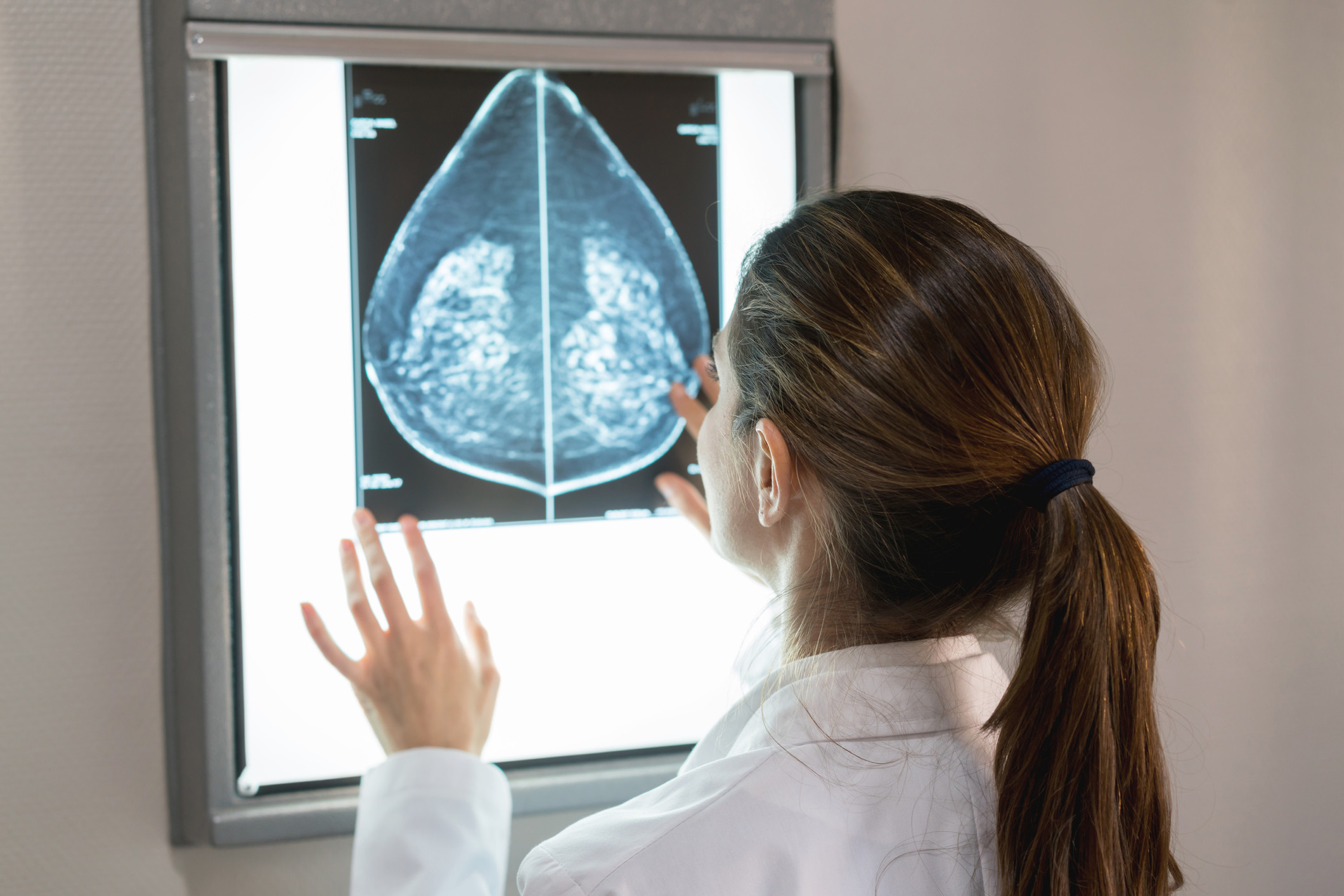
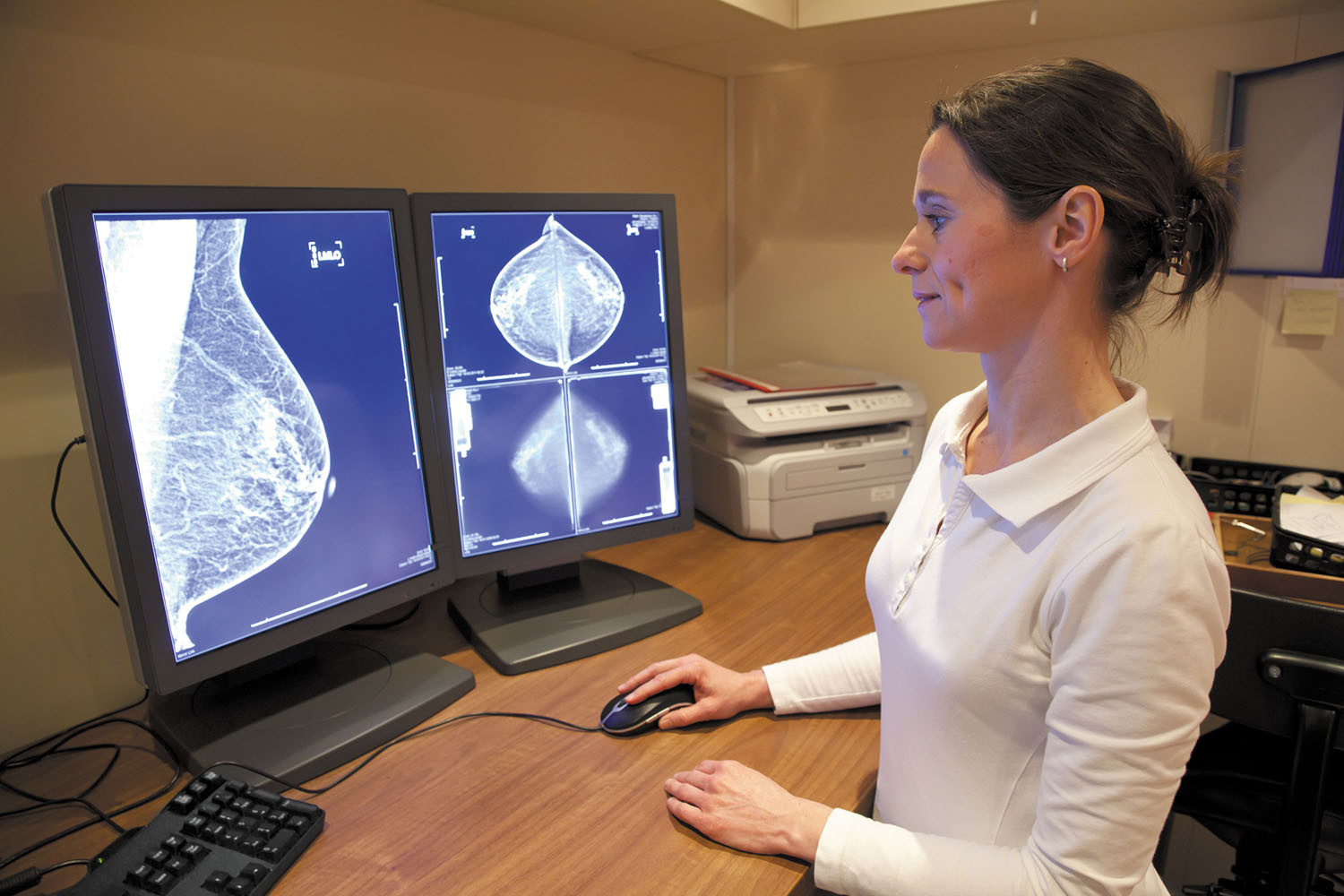
Can a new breast screening technology find more cancers in women with dense breast tissue? A study managed by the American College of Radiology (ACR) Center for Research and Innovation will compare contrast-enhanced spectral mammography (CESM) to other screening technologies used for dense breasts (those that contain a higher proportion of active tissue than fat). It's difficult to find cancers in dense breast tissue using traditional mammography because the active tissue shows up as white areas on a mammogram, just like cancers do, making abnormalities harder to see.
CESM is similar in some ways to traditional mammography, but before having the usual x-ray, the woman is injected with a special iodine-based contrast agent that highlights abnormal areas on the image more clearly. Cancerous tumors typically create new blood vessels when they form, and the contrast agent can reveal that increased blood flow, alerting the radiologist to a potential cancer.
Could your breast implants be making you sick?
Many women are reporting symptoms they believe are associated with their breast implants. Sometimes called breast implant illness, this combination of vague symptoms—such as hair loss, fatigue, anxiety, and depression—is also associated with a number of other conditions, including menopause, thyroid problems, and autoimmune conditions. Researchers are now working with patient advocacy groups to better understand the problem. Experts recommend that women understand the potential risks and benefits of breast implants before having the surgical procedure.
Hormones and breast cancer: What you should know
New research again links increased breast cancer risk to longer use of hormone therapy.
The link between hormone therapy and breast cancer has been recognized for years. But an analysis published Aug. 29, 2019, in The Lancet has added some additional information to the discussion. The analysis looked at 58 studies that included information on the type and timing of hormone use in individual women, and their body mass index. Researchers began gathering the studies in 1992 and continued until 2018.
We asked Dr. Wendy Chen, an assistant professor of medicine at Harvard Medical School, to help us sort through both the old and new information on hormone use and breast cancer and what it means for women considering starting hormone therapy.
Gene tests for all women with breast cancer could save money — and lives
Research we're watching
Doing genetic tests on all women with breast cancer, as compared with the typical practice of just testing those with a family history of the disease, is worth the extra cost, according to a study published online Oct. 3, 2019, by JAMA Oncology. The study authors say their findings should prompt the expansion of genetic testing to all women diagnosed with breast cancer. It's clear that testing breast cancer patients for genetic variants that raise breast cancer risk (such as BRCA1, BRCA2, and PALB2) would enable doctors to identify more women who carry these variants and who might benefit from preventive strategies. But researchers wondered whether doing so would be too costly. To answer that question, they used a computer model to analyze data from more than 11,000 women. They found that not only would the cost of testing all American women with breast cancer be balanced out by later savings on health care services, but also that just one year of testing could prevent an estimated 9,700 new cases of breast and ovarian cancer and 2,400 deaths.
Image: voinSveta/Getty Images
High risk for breast cancer? You might benefit from preventive medication
Research we're watching
Women at high risk for breast cancer might benefit from taking medication to prevent the disease, says a new recommendation from the U.S. Preventive Services Task Force (USPSTF), a national group of experts. Medications such as tamoxifen (Nolvadex), raloxifene (Evista), and aromatase inhibitors have been shown to help prevent invasive, estrogen receptor-positive breast cancer, but they can cause serious side effects, such as other cancers and blood clots. For some women, the potential benefits of these drugs outweigh those risks. The USPSTF, however, recommends against routine use of these medications for women who are not at high risk for breast cancer, because the potential benefit is much smaller. Women who are over age 35 and are at high risk for breast cancer or who have had previous benign breast lesions (such as atypical ductal or lobular hyperplasia or lobular carcinoma in situ) might want to discuss this recommendation with their doctor. The USPSTF encouraged doctors to weigh the risk of breast cancer against potential drawbacks of the medications and the individual woman's risk for adverse effects.
Image: ShutterOK/Getty Images
Dense breasts on a mammogram? What to know and do
Mammograms look for signs of breast cancer. They can also provide information on whether a woman has high breast density, which slightly increases risk for developing breast cancer. Here’s what you need to know and do if you’re notified about this risk factor.
Dealing with high-density breasts
The FDA may require mammography facilities to notify patients about this breast cancer risk factor, but women don't know what to do with this information.
Do you know how dense your breasts are? If you don't, a new proposal by the FDA may mean you will soon find out.
The agency proposed a change that, if approved, will require mammography facilities to send letters informing women about their breast density — a measure of the proportion of active tissue versus fat in their breasts (see "The FDA proposal").
Breast disorders in men
The male breast is much smaller than its female counterpart, and it cannot produce milk. Because of this smaller size and simpler structure, breast disease is much less common in men than women. Still, men can develop important breast problems, both benign and malignant. Early detection is the key to a successful outcome, so every man should understand the basic elements of male breast disease.
Jogger's nippleIrritation of the nipple is more common than enlargement of the breast itself. Pain, redness, and even bleeding of the male nipple are fairly common complications of intense, prolonged exercise — hence the common names "jogger's" and "marathoner's" nipple. The cause is not running itself but the mechanical irritation of the runner's shirt rubbing up and down against his chest, especially in hot, humid weather. You don't have to give up running to cure jogger's nipple. Instead, apply some petroleum jelly to your nipples before you run. Plastic Band-Aids are even better; round "spots" are particularly handy. Or simply run without a shirt when it's hot or humid. |
Newer breast screening technology may spot more cancers
Digital breast tomosynthesis may also reduce the number of unnecessary and nerve-racking callbacks for additional testing.
If you're in your 40s, you may want to consider switching from digital mammography to digital breast tomosynthesis (DBT) for your next breast cancer screening, say the authors of a study published online February 28 by JAMA Oncology.
A review of more than 170,000 screening mammograms using the two technologies determined that DBT — sometimes referred to as 3D mammography — did a better job at accurately detecting cancers in women of all ages. The advantages were most pronounced for women in their 40s. DBT was also better at finding cancers in women with high breast density, which can make cancers more difficult to spot on screening exams. High density indicates a larger proportion of active tissue in the breast and is a risk factor for breast cancer.

How high blood pressure harms your health

Time for a medication check-up?

Risk factors for MCI and dementia

Handling tough decisions as a caregiver

How we make memories

Treating mild cognitive impairment

Are you at risk for high blood pressure?

Cholesterol's various forms

Stopping a medication?

How to fall without injury
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up