Respiratory health harms often follow flooding: Taking these steps can help

Tips to leverage neuroplasticity to maintain cognitive fitness as you age

Can white noise really help you sleep better?

Celiac disease: Exploring four myths

What is prostatitis and how is it treated?

What is Cushing syndrome?

Exercises to relieve joint pain

Think your child has ADHD? What your pediatrician can do

Foam roller: Could you benefit from this massage tool?

Stepping up activity if winter slowed you down
Medical Tests & Procedures Archive
Articles
When the heart pumps normally but struggles
Ask the doctor
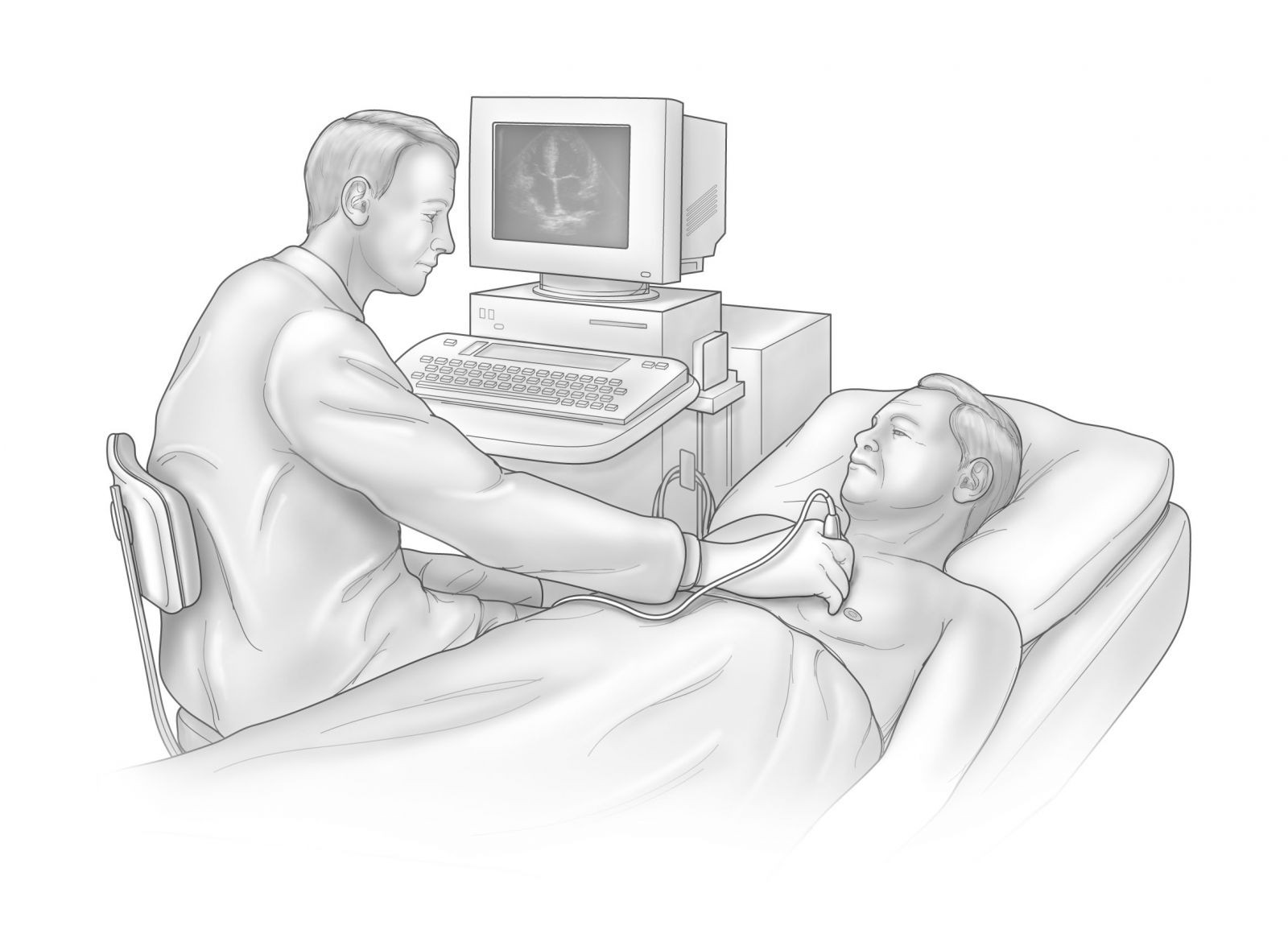
Illustration by Scott Leighton
Q. I was recently admitted to the hospital with heart failure and received a heart ultrasound. The test report stated that my heart's pumping ability is normal. I don't understand. Was my diagnosis wrong, or is the test wrong?
A. If you were diagnosed with heart failure in the hospital, I'm presuming that you were admitted with symptoms such as shortness of breath, fatigue, and difficulty doing everyday activities. Other common symptoms include swelling in your legs and feet and trouble breathing at night.
Does prostate cancer screening matter?
The latest guidelines suggest you should have an engaged conversation with your doctor about PSA testing.
Image: © Mark Bowden/Thinkstock
An annual prostate-specific antigen (PSA) test to check for signs of possible prostate cancer sounds innocent enough, but new guidelines suggest the test offers few long-term benefits, and substantial possible harm.
The updated guidelines from the U.S. Preventive Services Task Force (USPSTF), published online April 11, 2017, by The Journal of the American Medical Association, reinforce the organization's 2012 conclusion that PSA screenings have only a small potential benefit for reducing the chance of dying of prostate cancer for men ages 55 to 69 — while exposing them to possible overtreatment and side effects from biopsies, radiation, and surgery.
Clot prevention with a mechanical heart valve
Ask the doctor
Image: © Hailshadow/Thinkstock
Q. I have a mechanical heart valve, so I'm taking warfarin. But the frequent blood tests and occasional dose changes are bothersome. When, if ever, will I be able to take one of the new blood thinners instead of warfarin? Off-label use of other drugs is not uncommon. Why isn't that an option in this case?
A. Your question is a good one, and it requires a two-part answer. When doctors prescribe drugs "off-label," that means they believe the drug will help you, even if it has not been FDA-approved specifically for your condition. Sometimes, subsequent research provides strong evidence to support a specific off-label use, which may lead to the drug's FDA approval for that condition. But sometimes, research shows the exact opposite: a medication that doctors assumed would be beneficial is, in fact, not helpful — and sometimes even harmful.
Is advanced lipoprotein testing useful?
Ask the doctor
Image: © designer491/Thinkstock
Q. I'm a trim, healthy 57-year-old who exercises religiously, six days a week. I take a low-dose statin and my cholesterol numbers are pretty good (total cholesterol is 146, LDL is 77, and HDL is 51). But a recent blood test showed that my lipoprotein subfractions are not ideal: my small LDL and large HDL values are considered "high risk," according to the report I received. What can I do to improve my lipoprotein subfractions, and how important are they in the overall scheme of things?
A. It sounds like you had advanced lipoprotein testing, which is a more detailed and also more expensive version of a standard cholesterol or lipid test. In general, I'm not a fan of this type of testing, because there is no solid evidence that the results are useful in any concrete way or provide information that can improve a person's health. To understand why, a little background on cholesterol and its role in heart disease may be of help.
Putting the brakes on a racing heart
A rapid heartbeat can be frightening, but this often-fleeting problem is usually harmless.
Image: © deeepblue/Thinkstock
If you're exercising or feeling very nervous, you expect your heart to beat faster than normal. But what if your heart sometimes starts racing out of the blue, for no apparent reason? You might have supraventricular tachycardia, or SVT. SVT is an umbrella term that covers several different types of rapid heart rhythms, all of which are caused by an electrical glitch in the upper part of the heart.
The most common SVTs are atrial fibrillation — a rapid, chaotic rhythm that increases the chance of having a stroke—and atrial flutter, a fast but usually regular heartbeat. But when cardiologists talk about SVT, they're usually referring to three different, less-common conditions (see "What is supraventricular tachycardia?").
When does long-term acid reflux become a serious issue?
On call
Q. I have had acid reflux for many years, but it is well controlled with a proton-pump inhibitor. However, I am concerned about long-term damage from my reflux, even though I feel fine now. Should I have an upper endoscopy to look for possible damage?
A. Long-term acid reflux can damage the esophagus and may lead to a condition known as Barrett's esophagus, which is a precursor to esophageal cancer. Barrett's affects about 3% to 10% of older men, but within this group the risk of developing esophageal cancer is only about four in every 1,000 cases. Over all, men with Barrett's are more likely to die from another cause.
Scalp cooling reduces hair loss during breast cancer chemotherapy
Research we're watching
For many women with breast cancer, hair loss is the most distressing side effect of chemotherapy. Although cooling the scalp with ice packs has been tested, the technique has had limited success. However, a newer approach — wearing a cap connected to a cooling system that gradually reduces scalp temperature — has been more successful, according to two reports in the Feb. 14, 2017, Journal of the American Medical Association.
In one study, 67 of 106 women with stage I or stage II breast cancer who used the FDA-approved DigniCap during their treatment with taxane (Taxol and others) lost less than half of their hair. In comparison, 16 women who underwent the same treatment but did not wear the cooling cap lost all of their hair.
Heart scans: Why and when you might consider one
Coronary artery calcium tests can reveal early signs of heart disease. But they're not appropriate for everyone.
Image: © Monkey Business Images/Thinkstock
A special x-ray scan can show specks of calcium inside the walls of the heart's arteries within a matter of minutes. Known as a coronary artery calcium (CAC) scan, it offers one way to predict a person's future risk of heart disease.
However, having this test makes sense only if the results would affect a person's medical treatment. For the most part, that means it's useful primarily for people who are wavering about whether to take a cholesterol-lowering statin drug, says Dr. Ron Blankstein, a cardiovascular imaging specialist and preventive cardiologist at Harvard-affiliated Brigham and Women's Hospital.
Does your heart need a valve job?
Because medications cannot effectively treat aortic stenosis, a stiff, narrowed aortic valve needs to be replaced.
Your aortic valve is the gateway between your heart and body. With every heartbeat, it opens to allow blood to flow to your body, then snaps shut to keep blood from moving back into the heart.
As people age, calcium deposits may collect on the hard-working aortic valve, causing it to stiffen and narrow. Known as aortic stenosis, this condition also can result from a genetic abnormality (see "What is a bicuspid aortic valve?"). But most cases are in older people, often — but not always — those with high blood pressure, high cholesterol, and other risk factors linked to heart disease. In the United States, about three to four of every 100 people ages 75 and older have severe aortic stenosis.
Blood markers for heart disease linked to microscopic strokes
Research we're watching
Aging brains often show signs of microscopic strokes, which result from damage to tiny blood vessels within the brain. Those that occur in the brain's outermost layer — called cortical cerebral microinfarcts (CMIs) — usually don't cause any symptoms. But they are more common in autopsies of people diagnosed with dementia. Now, new research suggests a link between blood markers for early heart disease and CMIs.
The study, published online Feb. 6, 2017, by JAMA Neurology, included 243 people who attended a memory clinic. All had brain scans to check for CMIs and blood tests that measured two substances associated with early signs of heart damage. People who had CMIs (nearly 29% of the participants) were much more likely to have heart disease than those who didn't have CMIs. Higher levels of both substances associated with heart damage were also linked to CMIs — even when the researchers left out people who already had obvious symptoms of heart disease.

Respiratory health harms often follow flooding: Taking these steps can help

Tips to leverage neuroplasticity to maintain cognitive fitness as you age

Can white noise really help you sleep better?

Celiac disease: Exploring four myths

What is prostatitis and how is it treated?

What is Cushing syndrome?

Exercises to relieve joint pain

Think your child has ADHD? What your pediatrician can do

Foam roller: Could you benefit from this massage tool?

Stepping up activity if winter slowed you down
Free Healthbeat Signup
Get the latest in health news delivered to your inbox!
Sign Up